Atrial Septal Defect (ASD)

What is it?
An atrial septal defect (ASD) is an abnormal opening or hole in the septum—the muscular wall that separates the heart’s two upper chambers, known as the atria. This wall normally keeps oxygen-rich blood on the left side of the heart separate from oxygen-poor blood on the right side.
When an ASD is present, oxygen-rich blood from the left atrium leaks into the right atrium. As a result, excess blood flows into the right side of the heart and is repeatedly sent to the lungs. Over time, this abnormal circulation can cause enlargement of the right atrium and right ventricle, increased blood flow to the lungs, and strain on the pulmonary blood vessels.
Although some small defects may remain silent for years, larger ASDs can lead to breathlessness, easy fatigue, recurrent chest infections in children, abnormal heart rhythms, pulmonary hypertension, or heart failure later in life if left untreated. ASD is a congenital heart defect, meaning it is present from birth, and its severity depends on the size of the opening and the amount of blood shunting across the septum.
What causes it?
Before birth, every baby has a natural opening between the two upper chambers of the heart. This opening allows blood to bypass the lungs, which are not yet functioning while the baby is in the womb. After birth, once the lungs begin to work, this opening is no longer required and normally closes on its own or becomes very small within the first few weeks or months of life.
In some cases, the opening remains larger than normal and fails to close after birth. When this happens, it is referred to as an atrial septal defect (ASD). In most children, the exact cause of this condition is unknown. Occasionally, ASD may occur along with other congenital heart abnormalities.
How does it affect the heart?
Under normal conditions, the left side of the heart pumps oxygen-rich blood to the rest of the body, while the right side pumps oxygen-poor blood to the lungs. In a child with an atrial septal defect (ASD), blood can pass through the opening in the septum, moving from the left atrium into the right atrium and then being directed back to the lungs.
When the defect is large, this extra blood flow to the lung arteries forces both the heart and the lungs to work harder than normal. Over time, this increased workload can lead to enlargement of the right side of the heart and gradual damage to the lung blood vessels.
If the opening is small, it may cause little or no symptoms and may not lead to significant problems. In fact, many healthy adults have a small residual opening between the atria, known as a Patent Foramen Ovale (PFO), which often remains harmless and unnoticed throughout life.
How does the ASD affect my child?
Many children with an atrial septal defect (ASD) do not show any noticeable symptoms. When the defect is small, it usually causes no problems because the heart and lungs are not placed under additional strain. In cases where the opening is larger, the only detectable sign may be a heart murmur or other unusual heart sounds heard during examination with a stethoscope.
The greatest concern in children with a large ASD is the effect on the blood vessels of the lungs. Because an increased volume of blood is directed to the lungs, these vessels are exposed to higher flow over time. If left untreated, this prolonged overload—typically developing over many years—can lead to irreversible damage to the lung blood vessels.
Can the ASD be repaired with Device or Surgery?
If the opening in the heart is small, it usually does not put extra strain on the heart or lungs, so surgery or other treatments may not be necessary. Small ASDs found in infants often close or become smaller on their own. There is no medication that can make an ASD shrink or close faster than it naturally would.
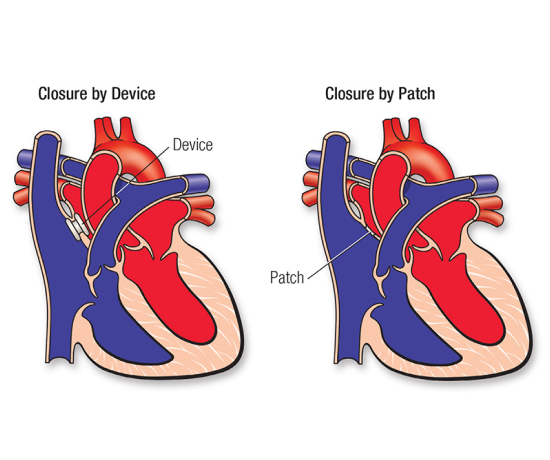
However, if the ASD is large, it may need to be closed either through open-heart surgery or by cardiac catheterization, in which a device is inserted to plug the opening. In some cases, if the ASD is in an unusual location or if other heart abnormalities are present—such as abnormal pulmonary vein connections—the catheter method cannot be used, and surgery becomes necessary.
Open-heart surgery to close a large ASD is often performed in early childhood, even in children with minimal symptoms, to prevent complications later in life. Many of these defects can be closed with sutures alone, without the need for a patch.
What activities can my child do?
Your child might not require any special precautions and can often take part in regular activities without added risk. Following surgery or catheter closure, the pediatric cardiologist may recommend temporary adjustments to activity. Once your child has fully recovered from the procedure, most children have no activity restrictions. In some cases, medication may be prescribed for a few months to prevent blood clots or infections after ASD closure.
What will my child need in the future?
Depending on the type of ASD, your child’s pediatric cardiologist may schedule periodic check-ups to monitor for any rare complications. After surgery to close the ASD, regular follow-up visits are required for a short period. The long-term outlook is very good, and most children do not need ongoing medication or additional surgery or catheter procedures.
If I had surgery to close an ASD in childhood, what can I expect?
A large ASD is often closed in early childhood, even if the child shows few symptoms, to prevent future complications. Some defects are closed using a patch made from the heart’s natural lining (pericardium) or synthetic materials like Dacron, while many can be sewn closed without a patch. The outlook after ASD closure in childhood is excellent, and long-term complications are rare.


